Table of Contents
Introduction
An allergic reaction can turn a normal day upside down in an instant. Whether it’s a runny nose, itchy skin, or something more serious, knowing the causes, symptoms, and treatments of allergies can help you take control before things escalate. Read on to discover how to protect yourself and manage your symptoms effectively!
what is allergic reaction?
An allergic reaction is an overreaction of the immune system to a substance (known as an allergen) that is typically harmless to most people. When someone with allergies is exposed to an allergen, their immune system mistakes it for a harmful substance and releases chemicals like histamine to protect the body. This can lead to symptoms like itching, swelling, hives, runny nose, sneezing, difficulty breathing, or even more severe reactions like anaphylaxis.
Common allergens include:
- Pollen
- Pet dander
- Certain foods (e.g., peanuts, shellfish)

Types of allergic reactions (hypersensitivity)
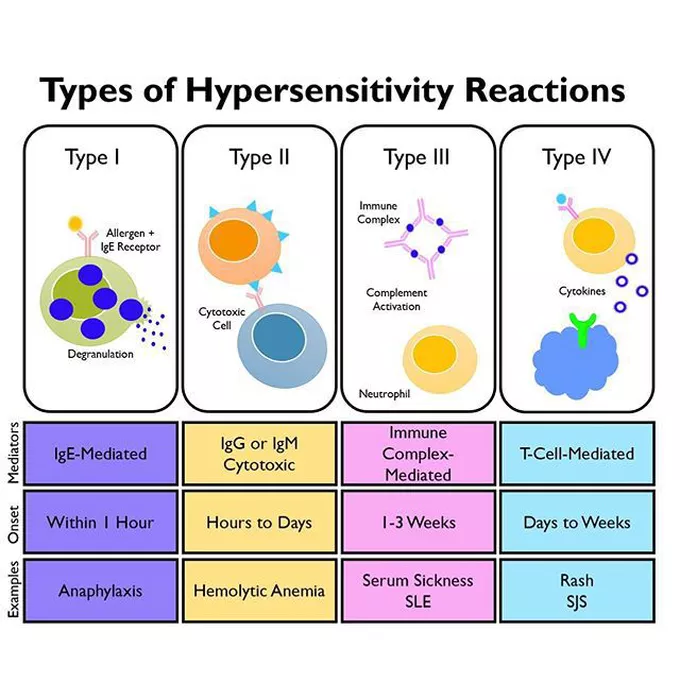
- Type 1 reactions are severe and occur rapidly, such as with allergies to penicillin, latex, or peanuts (e.g., IgE-mediated anaphylaxis). These reactions can be life-threatening and require immediate recognition and action to prevent serious harm.
- type 2 reactions are antibody-mediated and are typically not triggered by dental materials or drugs. Instead, they are often seen in autoimmune conditions affecting the oral cavity, such as pemphigus.
- type 3 reactions are immune complex-mediated and can occur due to dental materials, though they are more commonly triggered by viral infections, such as recurrent herpes labialis. These reactions can lead to conditions like erythema multiforme or Stevens-Johnson syndrome.
- Type 4 reactions are cell-mediated or delayed hypersensitivity reactions, commonly seen in response to dental materials. These reactions typically occur in the oral cavity, where materials like amalgam or gold restorations are in direct contact with the buccal or lingual mucosa.
Summary
- Type 1 reactions are acute and require immediate action, like with penicillin or peanut allergies.
- Type 2 involves antibody-mediated responses, often linked to autoimmune conditions like pemphigus.
- Type 3 is immune complex-mediated, seen in reactions to dental materials or viral infections.
- Type 4 is cell-mediated, commonly causing contact sensitivity to dental materials like amalgam or gold.
Type I allergic Reactions (Hypersensitivity)
- Type I reactions, also known as anaphylaxis, are severe allergic reactions that happen very quickly.
- This condition affects the whole body and can cause serious symptoms in many parts of the body all at once.
- If not treated immediately, anaphylaxis can be fatal because it can quickly lead to trouble breathing and even collapse.
Allergic reaction mechanisms (Pathophysiology )
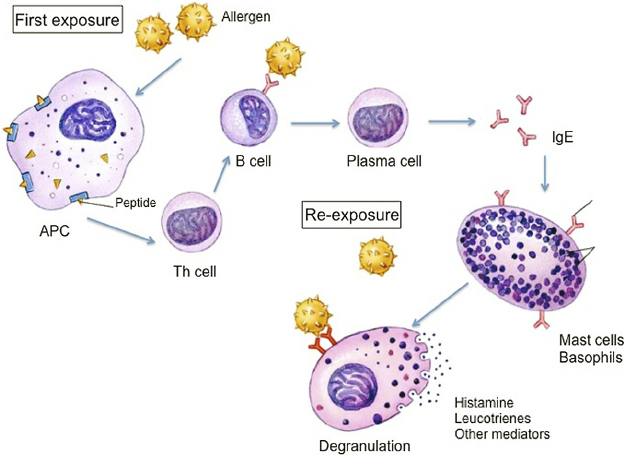
How Mast Cells and IgE Trigger Allergic Reactions
- Reactions happen when certain cells in your body, called mast cells, have special molecules (called IgE) attached to them. These cells are ready to react when they come into contact with something harmful or an allergen, like pollen or pet dander. When the mast cells are triggered, they release substances that cause the reaction, like itching or swelling.
- A patient who has been exposed to a drug or other substance before will have antibodies, primarily IgE, attached to their mast cells. This makes the mast cells sensitive to that substance, so when they encounter it again, they trigger a reaction.
- When the antigen, whether it’s a drug, food, or airborne substance, re-enters the body, it binds to the antibodies on the mast cells, causing them to link together. This triggers a reaction from the mast cells.
The Effects of Mast Cell Activation on the Body
- This binding triggers an increase in calcium inside the mast cells, which leads to the release of stored substances, including histamine, proteases, leukotrienes, and prostaglandins.
- Along with these substances, the body also releases signals called cytokines. These signals attract eosinophils, a type of white blood cell, which help increase the inflammation. As a result, blood vessels expand and become more leaky, causing fluid and immune cells, like eosinophils, to build up in the tissues, leading to swelling.
- When IgE antibodies bind to mast cells in the lungs, it causes the muscles around the airways to tighten, making it harder to breathe. The allergic reaction can be localized, causing symptoms like hives (urticaria) or swelling under the skin (angioedema), but it can also spread throughout the body, leading to a serious reaction called anaphylactic shock.
Summary
Mast Cells & IgE: IgE antibodies on mast cells make them react to allergens, releasing chemicals like histamine.
Triggering Reaction: When an allergen binds to IgE, mast cells release substances causing inflammation and symptoms.
Inflammation: These substances attract eosinophils, leading to swelling and fluid buildup in tissues.
Airway & Anaphylaxis: In the lungs, it tightens airways, causing difficulty breathing; severe reactions can lead to anaphylaxis.
Allergic reaction identification (Diagnosis)
Anaphylaxis is diagnosed based on symptoms and a doctor’s assessment, so lab tests or other diagnostics are usually not needed. Most deaths from anaphylaxis happen within the first hour after exposure to the trigger (the allergen).
Anaphylaxis should be considered if two or more systems, such as the skin, respiratory system, gastrointestinal system, or cardiovascular system, are affected, even if there’s no airway involvement or hypotension (low blood pressure)
Clinical Criteria for Anaphylaxis (1 of the following with onset within minutes to hours)*
Unknown exposure to an antigen yet rapidly developing urticaria or other skin/mucosal layer symptoms associated with any one of the following:
- Respiratory symptoms, such as difficulty breathing (dyspnea), wheezing, noisy breathing (stridor), low oxygen levels (hypoxemia), or trouble keeping the airways open, are warning signs. Persistent coughing or frequent throat clearing can also be early signs.
- Low blood pressure (hypotension), where the systolic pressure drops below 90 mm Hg or falls by more than 30% from a person’s usual levels, is another important sign of anaphylaxis.
- Signs of end-organ dysfunction, such as weakness (hypotonia), fainting (syncope), or loss of bladder control (incontinence), are also important indicators of anaphylaxis.
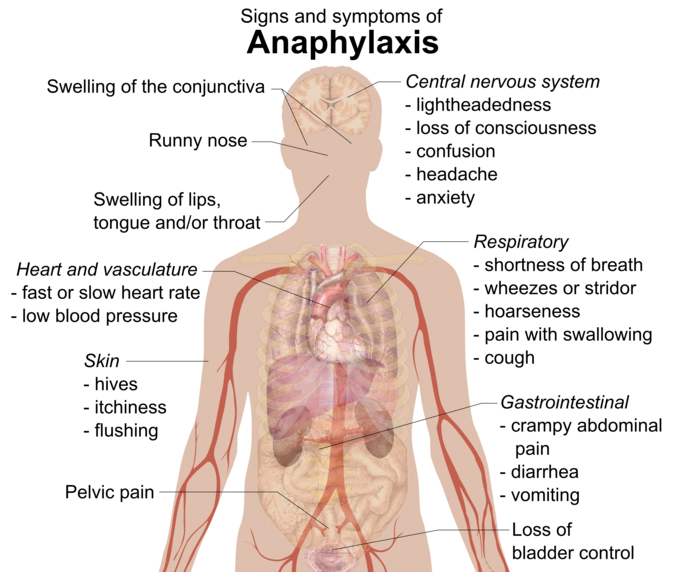
Key Indicators and Symptoms of Anaphylaxis
Possible exposure to an allergen, along with symptoms affecting at least two of the following body systems, is a key indicator of anaphylaxis:
- Integumentary symptoms such as a rash, itching (pruritus), redness (erythema), hives, or swelling of the face, lips, tongue, or uvula are common signs of anaphylaxis.
- Respiratory symptoms, such as difficulty breathing (dyspnea), wheezing, noisy breathing (stridor), low oxygen levels (hypoxemia), or trouble keeping the airways open, are common signs of anaphylaxis. Persistent coughing or frequent throat clearing can also be early warning signs.
- Hypotension, where systolic blood pressure drops below 90 mm Hg or decreases by more than 30% from the person’s normal levels, is a key sign of anaphylaxis.
- Gastrointestinal symptoms: persistent, painful cramps or vomiting
Angioedema can resemble anaphylaxis, but the main difference is the presence of hives (urticaria) in anaphylaxis. Both conditions can cause similar symptoms in the mouth and may require airway management. If you’re unsure, it’s important to treat aggressively to avoid serious complications.
“Kounis syndrome, also known as allergic angina, is a condition where a heart attack (myocardial infarction) or reduced blood flow to the heart (ischemia) occurs during anaphylaxis.
Summary
Diagnosis: Anaphylaxis is diagnosed based on symptoms, with most deaths occurring within an hour of allergen exposure.
Symptoms: Two or more affected systems (skin, respiratory, gastrointestinal, cardiovascular) suggest anaphylaxis.
Key Signs: Symptoms include hives, difficulty breathing, low blood pressure, and gastrointestinal issues.
Related Conditions: Angioedema and Kounis syndrome (heart issues) can occur during anaphylaxis.
Allergic reaction treatment
Airway
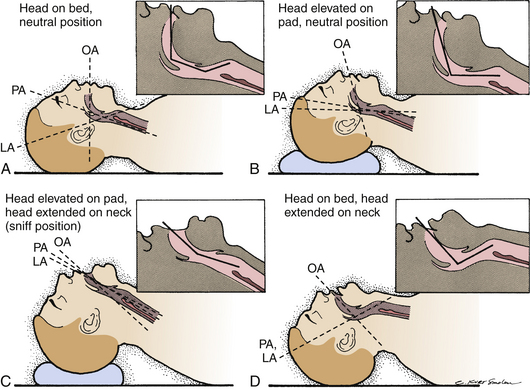
During an anaphylactic reaction, it’s crucial to manage the airway. Doctors will check if the airway is open and monitor for signs like perioral edema (swelling around the mouth), stridor (noisy breathing), or angioedema (severe swelling). If these occur, securing the airway quickly is necessary. Delaying this can cause further swelling, making it harder to insert a breathing tube and increasing the risk of needing a surgical airway to help the person breathe.
Summary
- Airway management: Vital during anaphylaxis to ensure proper breathing.
- Signs to monitor: Perioral edema, stridor, and angioedema indicate airway obstruction.
- Quick intervention: Securing the airway immediately prevents worsening of the situation.
- Risks of delay: Delaying action can lead to increased swelling and may require a surgical airway.
Decontamination
Once the airway is secured, the next priority is to remove any known offending agents to prevent further exposure and worsening of the reaction. If a stinger is present, it should be removed immediately. In cases of ingestion, gastric lavage should not be attempted, as it is usually ineffective and could delay other essential treatments.
Epinephrine
The next step is the administration of epinephrine. It is given via intramuscular (IM) injection at a dose of 0.3 to 0.5 mL of a 1:1,000 concentration for adults, and 0.01 mg/kg or 0.15 mg for children. While intravenous (IV) administration is faster, IM delivery of epinephrine is preferred because it provides more reliable absorption and better outcomes in anaphylaxis. If IV epinephrine is required, the concentration should be 1:10,000.
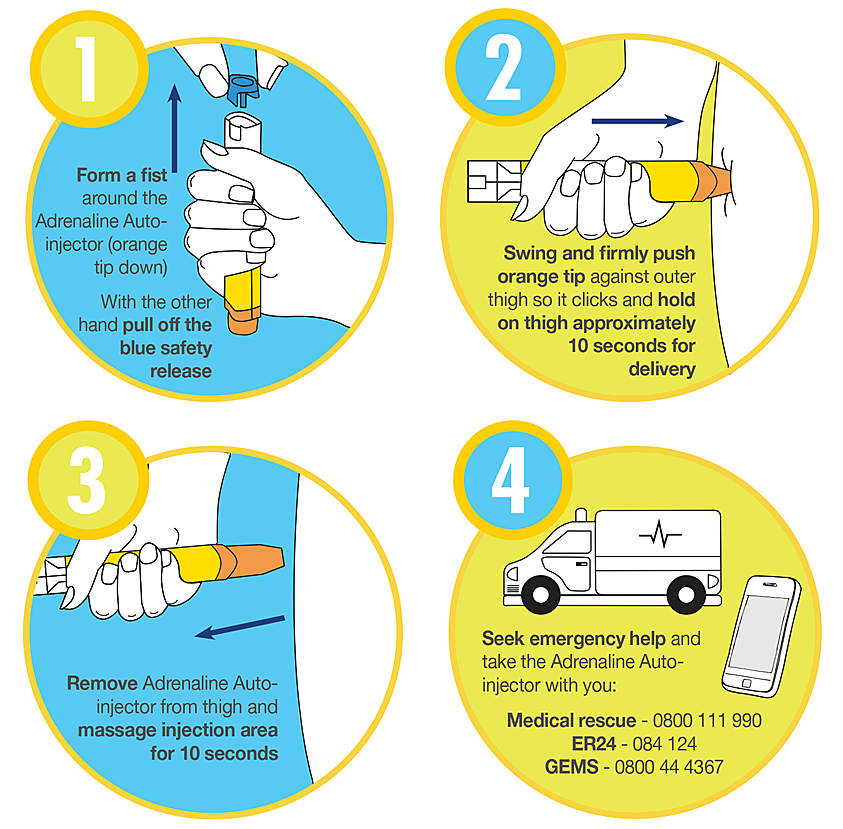
The thigh is the preferred site for injection over the deltoid, as it allows for quicker absorption. Studies have shown that providers often delay giving epinephrine, but it is the treatment of choice in anaphylaxis, and the rapid benefits far outweigh the risks of waiting. While most patients will only need one dose, repeat doses may be given every 5 to 10 minutes if symptoms persist, until improvement is seen.
Summary
- Epinephrine administration: Given IM at 0.3-0.5 mL (1:1,000) for adults, 0.01 mg/kg or 0.15 mg for children.
- IM vs IV: IM preferred for reliable absorption and better outcomes, although IV is faster with a 1:10,000 concentration.
- Injection site: Thigh preferred over deltoid for quicker absorption.
- Repeat doses: If symptoms persist, repeat every 5-10 minutes until improvement.
IV Fluid Resuscitation
IV fluid resuscitation is the next step if hypotension is observed, as anaphylaxis causes distributive shock that responds well to fluids. A bolus of 1 to 2 liters or 10 to 20 mL/kg of isotonic crystalloid should be given. Albumin or hypertonic solutions are not recommended for this situation. The goal is to restore circulation and stabilize the patient, supporting the effects of epinephrine.
Adjunctive Therapies
- When anaphylaxis is diagnosed, additional treatments may be started alongside epinephrine to support the patient’s recovery.
- These can include steroids, antihistamines, inhaled bronchodilators, and vasopressors. If necessary, glucagon can also be used.
- These medications help manage persistent symptoms, prevent recurrence, and reduce the risk of biphasic reactions (a second wave of symptoms after initial improvement).
- They are typically used in cases where the anaphylaxis is resistant to initial treatment or when ongoing support is needed.
Corticosteroids
- Corticosteroids are often administered to help reduce the duration of anaphylaxis or to prevent a biphasic response, where symptoms reappear after initial improvement.
- Although there is limited evidence specifically supporting their use in anaphylaxis, corticosteroids have been shown to be effective in treating reactive airway diseases.
- As a result, their use, dosages, and mechanisms of action follow similar protocols to those used in managing airway issues, aiming to reduce inflammation and prevent recurrence of symptoms.
- During the acute phase of anaphylaxis, corticosteroids like methylprednisolone (80 to 125 mg IV) or hydrocortisone (250 to 500 mg IV) are commonly used.
- Following the initial treatment, oral prednisone (40 to 60 mg daily, divided into two doses) is typically continued for 3 to 5 days.
- If the allergen source is unknown or there’s concern about a delayed follow-up, a steroid taper of up to 2 weeks may be considered.
- It’s important to note that corticosteroids like methylprednisolone and dexamethasone are preferred in patients at risk of fluid retention, as they have minimal mineralocorticoid activity compared to other steroids.
Summary
- Corticosteroid use: Reduces anaphylaxis duration and prevents biphasic reactions.
- Effectiveness: Limited evidence in anaphylaxis, but effective for reactive airway diseases.
- Common corticosteroids: Methylprednisolone (80-125 mg IV) or hydrocortisone (250-500 mg IV) in acute phase.
- Follow-up treatment: Oral prednisone (40-60 mg daily) for 3-5 days, with possible taper for up to 2 weeks.
Antihistamines
- Antihistamines, particularly H1 blockers like diphenhydramine (25 to 50 mg IV/IM), are commonly used in the management of anaphylaxis, although their clinical benefit specifically in anaphylaxis is not well-proven.
- However, they are helpful for less severe allergic reactions. In more severe cases, H1 blockers such as ranitidine (50 mg IV over 5 minutes) or cimetidine (300 mg IV) may also be used alongside H2 blockers, as there is evidence suggesting histamine can affect both types of receptors.
- It’s important to note that cimetidine should be used cautiously in patients with renal or liver impairment or those taking beta-blockers due to potential interactions.
- While IV administration is preferred initially for stabilization, patients may be switched to oral antihistamines once stabilized for continued treatment.
Summary
- Antihistamines (H1 blockers): Diphenhydramine (25-50 mg IV/IM) used in anaphylaxis, though benefit in severe cases is unproven.
- Severe cases: Ranitidine (50 mg IV) or cimetidine (300 mg IV) may be used alongside H2 blockers.
- Cimetidine caution: Use cautiously in patients with renal or liver impairment or those on beta-blockers due to interactions.
- Administration: IV preferred initially; oral antihistamines may be used once stabilized for ongoing treatment.
Bronchodilators
- Bronchodilators are valuable adjuncts in treating patients with bronchospasm, particularly those with a history of respiratory conditions such as asthma, as they are at higher risk during anaphylaxis.
- The first-line treatment for wheezing is inhaled beta-agonists like albuterol, which can also be combined with ipratropium bromide for additional benefit.
- If wheezing persists despite initial treatment, intravenous magnesium can be used, with dosing and management similar to that of severe asthma exacerbations, helping to relax the airways and improve breathing.
Summary
- Bronchodilators, like inhaled beta-agonists (albuterol), are key for treating bronchospasm and wheezing, especially in patients with asthma during anaphylaxis.
- If wheezing persists, intravenous magnesium can help relax airways and improve breathing, similar to severe asthma treatment.
Vasopressors
- Vasopressors may be used as an alternative when a patient requires additional doses of epinephrine but experiences unacceptable side effects, such as arrhythmias or chest pain, from the epinephrine IV infusion.
- If there is no clear second-line agent identified, treatment should follow standard guidelines for managing any patient in hypotensive shock.
- The goal is to stabilize blood pressure and support circulation while minimizing adverse effects.
Glucagon
- Glucagon is used as a reversal agent for beta-blockers and can be administered in cases where anaphylaxis is resistant to treatment in patients on beta-blockers.
- It helps to counteract the effects of beta-blockade, improving heart function and blood pressure.
- However, glucagon can cause side effects such as nausea, vomiting, hypokalemia (low potassium levels), dizziness, and hyperglycemia (high blood sugar).
- These side effects should be monitored and managed accordingly.
Different Conditions
1. Localized Anaphylaxis
- A localized allergic reaction that affects the small blood vessels can cause hives (also known as urticaria), which are raised, red bumps on the skin.
- Urticaria (hives) starts with itching (pruritus) in the area where histamine and other active substances are released.
- Swollen, raised areas (wheals or welts) then appear on the skin, usually on a red (erythematous) base with localized swelling (edema).
- These lesions can appear anywhere on the skin or mucous membranes (the moist lining inside the body, like in the mouth).
- There seems to be little doubt that the oral mucosa is rich in mast cells, and that type 1 allergic reactions can happen in the mouth.
- Urticaria (hives) on the lips and oral mucosa (the lining inside the mouth) most often occurs in allergic individuals after eating certain foods.
- Common food allergens that can trigger these reactions include chocolate, nuts, shellfish, and tomatoes.
- Drugs like penicillin and aspirin can trigger urticaria (hives), and in some people, cold, heat, or even pressure can cause the reaction.
- Impression compounds, coloring agents, preservatives, and even ingredients in mouthwashes can cause local swelling or, in some cases, anaphylaxis (a severe allergic reaction).
Summary
- A localized allergic reaction causes hives (urticaria), starting with itching and followed by raised, swollen areas on the skin.
- Urticaria can affect the skin or mucous membranes, often triggered by foods, medications, or environmental factors.
- Triggers include allergens like foods, drugs, and substances in mouthwashes, which can lead to swelling or severe allergic reactions (anaphylaxis).
2. Angioedema
- Rapid swelling, especially of the head and neck, often accompanied by hives (urticaria), can develop quickly.
- It happens when blood vessels deep in the subcutaneous tissue are affected, leading to a large, widespread area of swelling beneath the skin.
- Many patients experience short-term facial swelling that can be disfiguring, but if the edema (swelling) affects the neck and extends to the larynx (voice box), it can lead to life-threatening respiratory failure.
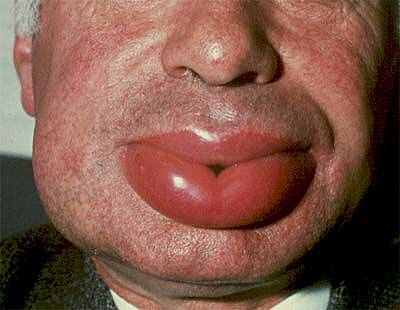
- Angioedema most often affects the lips, tongue, and around the eyes. It is usually temporary and not serious, unless swelling in the back of the tongue or larynx (voice box) interferes with breathing.
- Respiratory distress should be treated immediately with 0.5 mL of epinephrine (1:1000) injected under the skin (subcutaneously) or, preferably, into the muscle (intramuscularly). This can be repeated every 10 minutes until improvement begins.
- The patient should be given oxygen, laid down with their legs elevated (unless there’s a risk of breathing difficulty or vomiting), given fluids through an IV, and transported to the hospital immediately.
- Patients may need intubation to keep the airway open. Once the immediate danger has passed, 50 mg of diphenhydramine hydrochloride (Benadryl) should be given four times a day until the swelling goes down.
Summary
- Rapid swelling, especially of the head and neck, can occur with hives (urticaria) and may lead to life-threatening respiratory failure if the swelling affects the neck or larynx.
- Immediate treatment for respiratory distress includes epinephrine, oxygen, fluids, and transport to the hospital, where intubation may be needed.
- Once stabilized, patients should receive 50 mg of diphenhydramine (Benadryl) four times a day until the swelling subsides.
Type II Allergic Reactions
It is an antibody-mediated immune reaction in which antibodies (IgG or IgM) are directed against cellular or extracellular matrix antigens, resulting in cellular destruction, functional loss, or tissue damage. Damage can occur via three different mechanisms:
- Antibody binding to cell surface receptors and altering its activity
- Activation of the complement pathway
- Antibody-dependent cellular cytotoxicity
Etiology
- type II allergic reaction develops in response to cell surface modifications or matrix-associated antigens generating antigenic epitopes that are regarded as foreign by the immune system.
- The most common causes include medications like penicillin, thiazides, cephalosporins, and methyldopa.
- The drug molecule either binds to the surface of cells, resulting in a neoantigen, or alters the epitopes of the existing self-antigen on the cell surface.
- This directs the immune system to recognise modified antigens as foreign, leading to the breakdown of immune tolerance and the production of antibodies directed at self-antigens.
Immune tolerance is the phenomenon by which the immune system recognizes its antigens and does not generate an antibody response against its antigens. Factors that contribute to the breakdown of tolerance promote the production of antibodies against self-antigens
Pathophysiology
In type II allergic reactions, autoantibodies are produced (IgG and IgM) to the host cells (sensitization phase), promoting a series of pathogenic outcomes (effector phase).
The pathophysiology of type II allergic reactions can be broadly classified into three types:
- cell depletion or destruction without inflammation
- Inflammation mediated by complement or Fc receptor
- Cellular dysfunction by antibodies
The process involves a series of immune-mediated events that might take different forms
Cell Depletion or Destruction Without Inflammation:
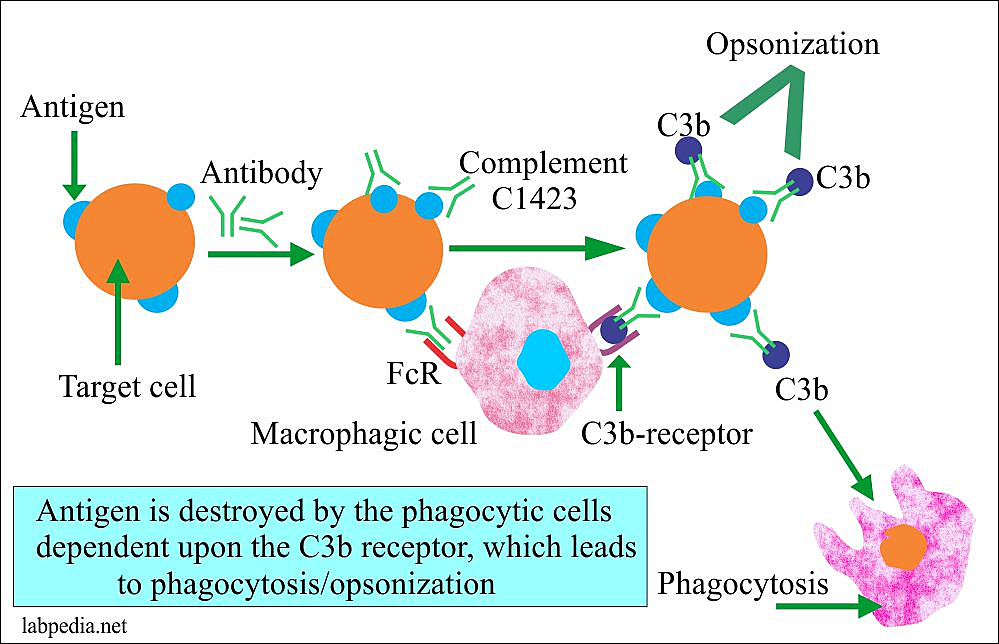
- Antibodies can bind to the target cell’s surface, particularly IgG antibodies.
- Through their Fc portion, they bind to their respective Fc receptor on the surface of macrophages and thus act as an opsonin. An opsonin is any molecule that enhances the phagocytosis of any substance.
- Thus by binding to both the target cell and the Fc receptor of the macrophage, it activates the macrophage and causes it to phagocytose the target cell.
- Antibodies can also bind to the target cell and activate the complement pathway resulting in the formation of complement component C3b.
- C3b which also acts as an opsonin and binds to the receptors on the surface of macrophages.
- This, in turn, activates the macrophages causing them to engulf the cell resulting in depletion of the cell.
Inflammation Mediated by Complement or Fc Receptor:
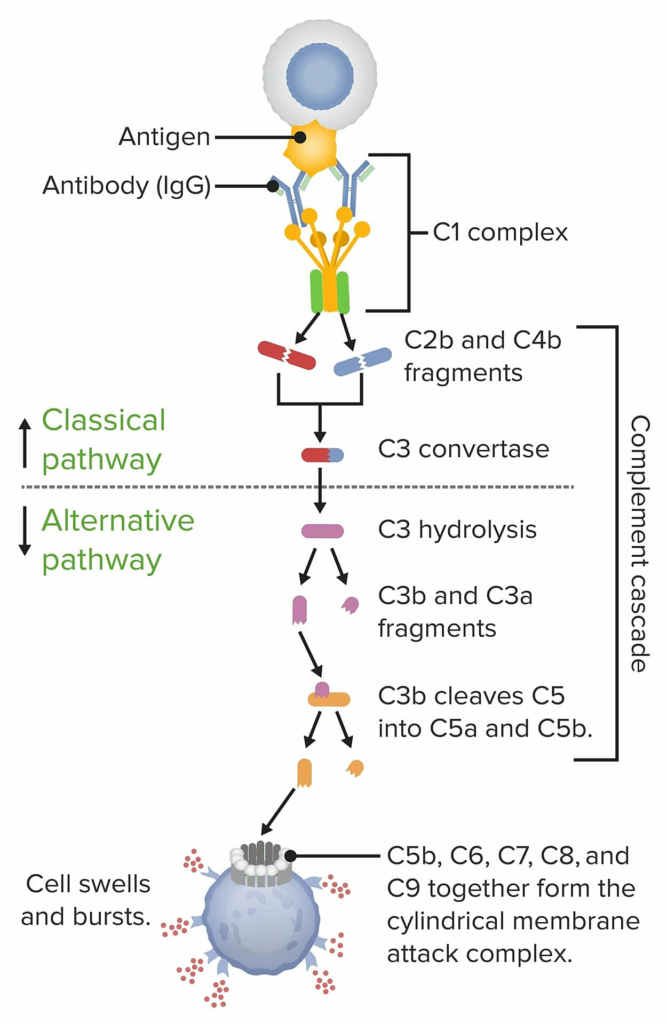
- Antibodies can activate the complement pathway by binding to self-antigens resulting in the formation of complement components C3a and C5a.
- C3a and C5a which act as chemotactic factors for neutrophils, causing the recruitment of neutrophils to the site and resulting in the activation of neutrophils.
- These neutrophils then release enzymes and reactive oxygen species, which damage the tissues.
- Antibodies against foreign antigens can also trigger complement activation and inflammation by a mechanism of molecular mimicry.
- This is the hallmark of acute rheumatic fever in which antibodies directed against streptococcal antigens structurally mimic cardiac myosin in the human heart, leading to cross-reactivity of these antibodies against bacterial and host antigens and therefore binding to the myosin and damaging the heart tissue.
Cellular Dysfunction by Antibodies
- Autoantibodies bind to the receptors on target cells, causing dysfunction without causing inflammation or destruction.
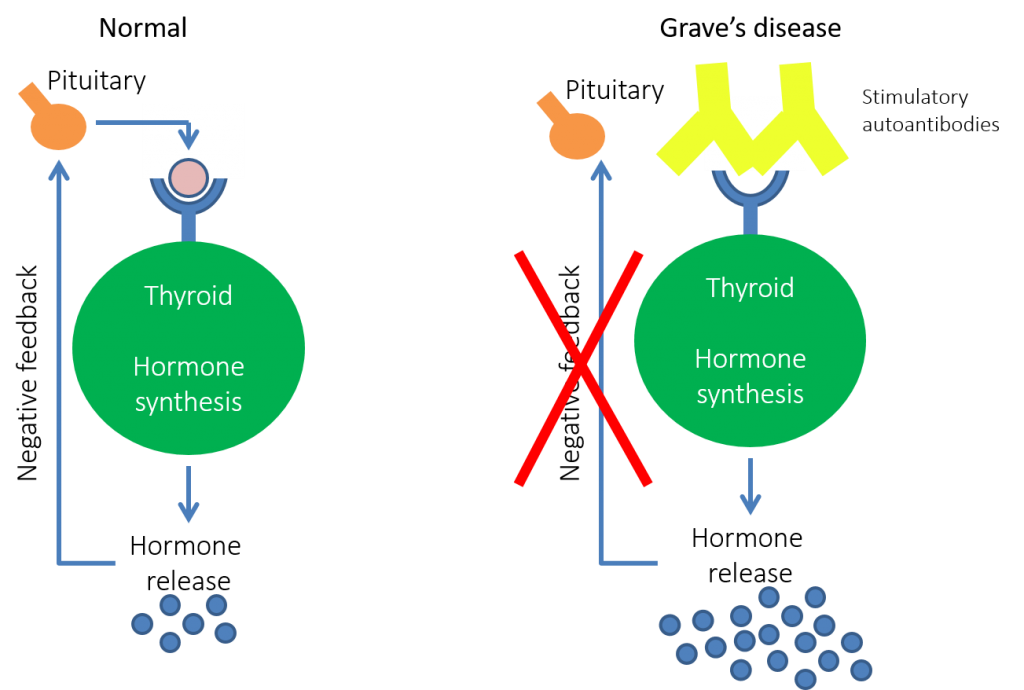
- example – in Graves disease, the autoantibodies bind to the thyrotropin receptor on thyroid follicular cells resulting in the overproduction of thyroid hormones.
- Normally, the production of thyrotropin by the pituitary is regulated by levels of thyroid hormones in the blood, but these antibodies lead to autonomous production of thyroid hormones by the follicular cells, which are not inhibited by high levels of thyroid hormones in the blood, resulting in much higher levels than cause symptoms of thyrotoxicosis
Symptoms
Signs and symptoms of type II allergic reactions include:
- thrombocytopenia and bleeding
- anemia
- bacterial and fungal infections
- neutropenia
- jaundice (in newborns)
- blistering skin
- extreme muscular fatigue
- double vision
- difficulty swallowing
Examples
Examples of type II allergic reactions include:
- rejection of an organ transplant
- Hashimoto thyroiditis
- Goodpasture syndrome
- hemolytic disease of the newborn
- myasthenia gravis
- pemphigus
- immune thrombocytopenia
- autoimmune hemolytic anemia
- autoimmune neutropenia
Diagnosis
- Doctors diagnose type II allergic reactions by confirming the presence of IgG and IgM antibodies through a blood test.
- Diagnosis is also based on your history and physical symptoms.
Treatment
- Immunosuppression is the main type of treatment for type II allergic reactions. For this, doctors often use systemic glucocorticoids to suppress the illness when it first appears or flares up.
- Intravenous immunoglobulin infusions are sometimes used to deliver human-derived antibodies to target the abnormal antibodies and neutralize them.
- Plasmapheresis, which is a procedure used to filter out a person’s antibodies and return clean blood to their body, is another possible treatment option for this type of hypersensitivity reaction.
Type III Allergic Reaction
Type III allergic reactions involve IgG antibodies binding to foreign antigens in the blood. This antibody-antigen complex gets stuck in certain locations—such as the blood vessels, skin, kidneys, or joints—and causes local damage.
Symptoms
Signs and symptoms of type III allergic reactions include:
- purpuras, which are small, non-blanching hemorrhages on the skin
- rheumatoid nodules
- a flushed rash on the face
- kidney damage
Examples
Examples of type III hypersensitivity reactions include:
- serum sickness
- rheumatoid arthritis
- systemic lupus erythematosus
- vasculitis
- glomerulonephritis
Treatment
- Treatment for type III allergicreactions involves immunosuppression, often using glucocorticoids.
- Disease-modifying antirheumatic drugs—such as methotrexate, cyclosporine, and cyclophosphamide—and biologic agents — such as TNF-blockers — are also used.
Diagnosis
- Diagnosing type III allergicreactions involves a medical history and physical exam based on your symptoms.
- There is no single test to identify the cause of this type of hypersensitivity reaction.
- Punch biopsies of vasculitis rashes can show whether or not there is local inflammation and tissue breakdown.
Type IV Allergic Reactions
Type IV allergic reactions do not involve antibodies. These are T-cell-mediated reactions that are activated by an antigen. Helper T cells recognize the antigen and send messengers that activate the immune system with killer T cells to destroy the target host.
This type of reaction occurs 48–72 hours after exposure to an antigen.
Symptoms
Symptoms of type IV hypersensitivity reactions include:
- an itchy rash
- flushed skin
- fever
- weakness
- weight loss
- skin vesicles with crust formation
- a decline in lung function
In some cases, such as with severe drug reactions, there is severe tissue damage and fluid loss that can result in hypovolemic shock. There may also be severe skin blistering that looks like a third-degree burn. In other cases, there is multiorgan involvement — particularly with the heart, lungs, kidneys, and liver.
Examples
The most common example of type IV hypersensitivity reaction is allergic contact dermatitis. The reaction that some people get to the Mantoux test, which is used to check for active tuberculosis, is also a form of type IV hypersensitivity.
There are also delayed drug reactions, including:
- Steven-Johnson syndrome (SJS)
- drug hypersensitivity syndrome
- erythema multiforme
- lichenoid drug eruptions
- morbilliform drug reactions
Diagnosis
- Doctors can diagnose these types of reactions using patch tests. With these tests, they apply a small number of potential allergens to the skin and leave them there for 2 days. If a patch of eczema forms at the site of exposure, the patch test is positive.
- A detailed medical history and physical exam are also required for an accurate diagnosis.
Treatment
- Avoiding the trigger allergen is the best form of treatment and prevention for type IV hypersensitivity reactions.
- For contact dermatitis, applying topical steroid creams can help manage skin symptoms. In the case of more severe allergic reactions, your doctor might prescribe oral corticosteroids and taper the dosage over a number of weeks.
- If SJS is present, acute care in a hospital with life saving treatment — such as fluid therapy and antibiotics — is warranted.
FAQs
Can allergic reaction cause fever?
Yes, an allergic reaction can sometimes cause a mild fever, especially if the body is responding to an infection or inflammation alongside the allergic response. However, fever is not a typical or primary symptom of allergies. More common symptoms include swelling, hives, itching, or respiratory issues. If you experience a high fever during an allergic reaction, it may indicate a more serious condition, and medical attention should be sought.
Can allergic reaction cause sore throat?
Yes, an allergic reaction can cause a sore throat. This can happen if the allergy triggers inflammation in the throat, especially if it’s associated with symptoms like post-nasal drip, which can irritate the throat. Additionally, if the allergic reaction involves the respiratory system, it may lead to swelling or irritation in the throat, causing discomfort or a sore throat. However, a sore throat is more commonly caused by viral or bacterial infections than by allergies alone.
Can allergic reaction cause coughing?
Yes, an allergic reaction can cause coughing. This often occurs when the allergens trigger inflammation in the airways, leading to irritation and coughing as the body tries to clear the irritants. Allergies affecting the respiratory system, such as hay fever or allergic asthma, can lead to symptoms like coughing, wheezing, and shortness of breath.
References
Okubo Y, Nochioka K, Testa MA. Nationwide Survey of Hospitalization Due to Pediatric Food-Induced Anaphylaxis in the United States. Pediatr Emerg Care. 2019 Nov;35(11):769-773. [PubMed]
Castilano A, Sternard B, Cummings ED, Shi R, Arnold T, Bahna SL. Pitfalls in anaphylaxis diagnosis and management at a university emergency department. Allergy Asthma Proc. 2018 Jul 01;39(4):316-321. [PubMed]
Akenroye AT, Ajala A, Azimi-Nekoo E, de Vos GS. Prevalence of anaphylaxis among adults admitted to critical care for severe asthma exacerbation. Emerg Med J. 2018 Oct;35(10):623-625. [PubMed]
Pattanaik D, Lieberman P, Lieberman J, Pongdee T, Keene AT. The changing face of anaphylaxis in adults and adolescents. Ann Allergy Asthma Immunol. 2018 Nov;121(5):594-597. [PubMed]
Mota I, Gaspar Â, Benito-Garcia F, Correia M, Chambel M, Morais-Almeida M. Drug-induced anaphylaxis: seven-year single-center survey. Eur Ann Allergy Clin Immunol. 2018 Sep;50(5):211-216. [PubMed]
Yue D, Ciccolini A, Avilla E, Waserman S. Food allergy and anaphylaxis. J Asthma Allergy. 2018;11:111-120. [PMC free article] [PubMed]
Parrish CP, Kim H. Food-Induced Anaphylaxis: an Update. Curr Allergy Asthma Rep. 2018 Jun 14;18(8):41. [PubMed]
Protudjer JLP, Olén O, Vetander M, Kull I, Melén E, van Hage M, Wickman M, Bergström A. Milk-Related Symptoms and Immunoglobulin E Reactivity in Swedish Children from Early Life to Adolescence. Nutrients. 2018 May 21;10(5) [PMC free article] [PubMed]
Anagnostou K. Anaphylaxis in Children: Epidemiology, Risk Factors and Management. Curr Pediatr Rev. 2018;14(3):180-186. [PubMed]
Jimenez-Rodriguez TW, Garcia-Neuer M, Alenazy LA, Castells M. Anaphylaxis in the 21st century: phenotypes, endotypes, and biomarkers. J Asthma Allergy. 2018;11:121-142. [PMC free article] [PubMed]
Valenta R, Karaulov A, Niederberger V, Gattinger P, van Hage M, Flicker S, Linhart B, Campana R, Focke-Tejkl M, Curin M, Eckl-Dorna J, Lupinek C, Resch-Marat Y, Vrtala S, Mittermann I, Garib V, Khaitov M, Valent P, Pickl WF. Molecular Aspects of Allergens and Allergy. Adv Immunol. 2018;138:195-256. [PubMed]
Graudins LV, Trubiano JA, Zubrinich CM, Elliott AS, Aung AK. Medication-related anaphylaxis treated in hospital: Agents implicated, patient outcomes, and management lessons. Pharmacoepidemiol Drug Saf. 2018 Sep;27(9):1029-1033. [PubMed]
Aun MV, Kalil J, Giavina-Bianchi P. Adults and children with anaphylaxis in the emergency room: why it is not recognized? Curr Opin Allergy Clin Immunol. 2018 Oct;18(5):377-381. [PubMed]
Navaradnam P, Suganthan N, Kumanan T, Sujanitha V, Mayorathan U. Kounis Syndrome and Multiorgan Failure Following Multiple Wasp Stings. Cureus. 2021 Apr 21;13(4):e14606. [PMC free article] [PubMed]
De Feo G, Parente R, Triggiani M. Pitfalls in anaphylaxis. Curr Opin Allergy Clin Immunol. 2018 Oct;18(5):382-386. [PubMed]
Cohen N, Capua T, Pivko D, Ben-Shoshan M, Benor S, Rimon A. Trends in the diagnosis and management of anaphylaxis in a tertiary care pediatric emergency department. Ann Allergy Asthma Immunol. 2018 Sep;121(3):348-352. [PubMed]
Gallagher JL, Rivera RD, Van Shepard K, Roushan T, Ahsan G, Ahamed SI, Chiu A, Jurken M, Simpson PM, Nugent M, Gobin KS, Wen CKF, Eldredge CE. Life-Threatening Allergies: Using a Patient-Engaged Approach. Telemed J E Health. 2019 Apr;25(4):319-325. [PubMed]
Jang HY, Ha DH, Rah SY, Lee DH, Lee SM, Park BH. Sirtuin 6 is a negative regulator of FcεRI signaling and anaphylactic responses. J Allergy Clin Immunol. 2022 Jan;149(1):156-167.e7. [PubMed]
Lindor RA, McMahon EM, Wood JP, Sadosty AT, Boie ET, Campbell RL. Anaphylaxis-related Malpractice Lawsuits. West J Emerg Med. 2018 Jul;19(4):693-700. [PMC free article] [PubMed]
Fineman SM. Optimal treatment of anaphylaxis: antihistamines versus epinephrine. Postgrad Med. 2014 Jul;126(4):73-81. [PubMed]
Leatherman BD. Anaphylaxis in the allergy practice. Int Forum Allergy Rhinol. 2014 Sep;4 Suppl 2:S60-5. [PubMed]
Rubin T, Clayton J, Adams D, Jou H, Vohra S. Systematic review of outcome measures in trials of pediatric anaphylaxis treatment. BMC Pediatr. 2014 Jun 20;14:158. [PMC free article] [PubMed]